Your foot strikes the ground approximately 625 times per km — that’s 20,000 foot strikes if you run 32K per week. With so many foot strikes, most of us can relate to running through some pain. And oftentimes, we convince ourselves to run through the pain instead of taking time off to give our bodies a break.
“Pain is a gift, it’s your body’s warning signal,” says Irene S. Davis, Ph.D., PT FACSM, director of the Spaulding National Running Center, in Cambridge, Massachusetts. “Running shouldn’t be painful.”
We spoke to Davis and Chelsea M. Evans, D.O., sports medicine specialist at the Lehigh Valley Health Network in Allentown, Pennsylvania, about how to identify nine basic foot injuries that plague runners, what causes them, and how to treat and prevent them. This guide is meant to help you identify and prevent issues, but as with any injury, it’s best to schedule a doctor’s visit to evaluate your injury and come up with a customized treatment plan for recovery.
Plantar Fasciitis
MT Stress Fracture
Morton’s Neuroma
Posterior Tibial Tendinitis
Peroneal Tendinitis
Achilles Tendinitis
Bunions
Metatarsalgia
Accessory Navicular Ankle Syndrome
Essential Terms
Sprain: a tear to the ligament connection from bone to bone.
Strain: an injury to a muscle.
Stress fracture: micro-fractures in the bone that accumulate over time; an imbalance of bone deposition, the formation of new bone, versus bone resorption, the breakdown of bone tissue.
Plantar Fasciitis
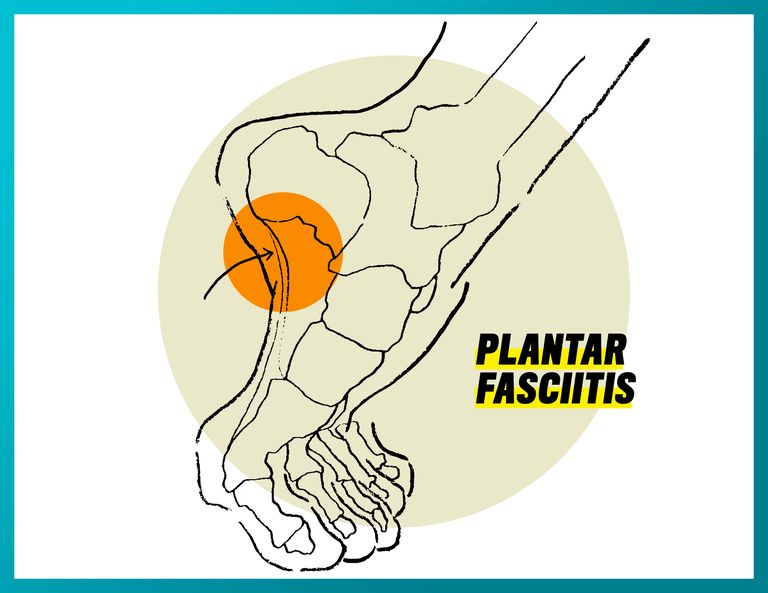
What it feels like: A searing pain in the arch that is often described as “like walking on glass” when you get out of bed in the morning. This is because your foot is plantar-flexed as you sleep; the tightened tissue becomes irritated when you stretch it as you take your first step in the a.m. The pain tends to alleviate midrun because the inflamed tissue is being stretched as you flex your foot. The pain eventually returns postrun, and the cycle continues.
What causes it: Plantar fasciitis is inflammation of the plantar fascia, a ligamentous type of connective tissue that extends from the heel to the base of the toes. And, this heel pain tends to strike those who overtrain, neglect to stretch their calf muscles, or overdo hill work and speedwork.
“It basically provides a restraint for the arch as you load (i.e., put pressure on your feet),” Davis says. “Every time you load, whether you’re walking or running, that plantar fascia gets stretched.”
Overtraining, or weak arch muscles, can result in overstretching the connective tissue and pain in the plantar fascia. Plantar fasciitis doesn’t discriminate; both high-arched and flat-arched runners are susceptible to this condition.
Evans also notes how the plantar fascia is a part of a kinetic chain; it starts at the heel attaching to the Achilles tendon, which means weak calf muscles could also be to blame.
Treatment and Prevention: Resting and icing your foot as well as orally taking anti-inflammatories will help lessen the pain, as it’s important to reduce swelling. Rolling a frozen water bottle under your foot can also help bring down inflammation. Rolling a tennis ball under your foot will loosen and massage your arch. Customized or over-the-counter devices, or taping as recommended by your doctor, can help calm it down. Once you wean it out of the device, Davis says, you’ll want to strengthen the muscles that support the plantar fascia.
Practicing calf and foot strengthening exercises is a proactive measure to stop plantar fasciitis from recurring.
MT Stress Fracture
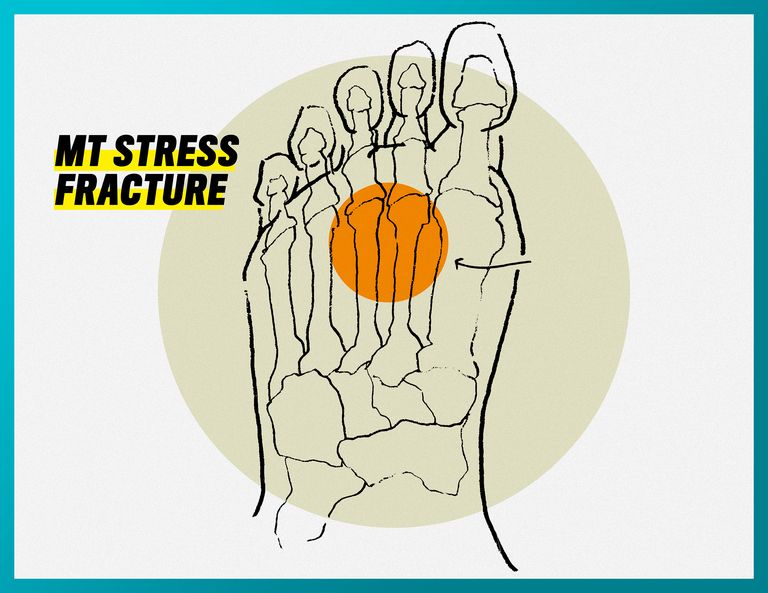
What it feels like: You feel the pain on the top of your foot while running, localized on the metatarsals, and feel no pain while resting. When the pain worsens it can carry over to walking. It can also be painful to the touch, or cause you to change your running stride.
What causes it: The metatarsals are the long bones in your foot. Of the five metatarsals, the second and third are most likely to fracture from running. Overstressing (i.e., jumping, dancing, running) the metatarsals can cause bone damage, which mends itself through resorption of the old bone and rebuilding of a new one. When new bone formation takes longer than resorption, the bone is susceptible to being fractured. People with long thin bones have a greater risk of developing stress fractures. Osteoporosis can also cause stress fractures.
The best way to truly know if you’ve fractured your metatarsals is by seeing a doctor for an MRI, as some stress fractures won’t show up on an X-ray.
Treatment/Prevention: Sufferers usually have to be placed in a walking boot for the bone to properly heal. Evans says it’s an eight-week process, with limited weight-bearing the first four weeks, and then weight-bearing, still in the boot, the next four weeks. After getting proper rest, practicing foot and calf exercises is recommended to strengthen your feet and legs.
Morton’s Neuroma
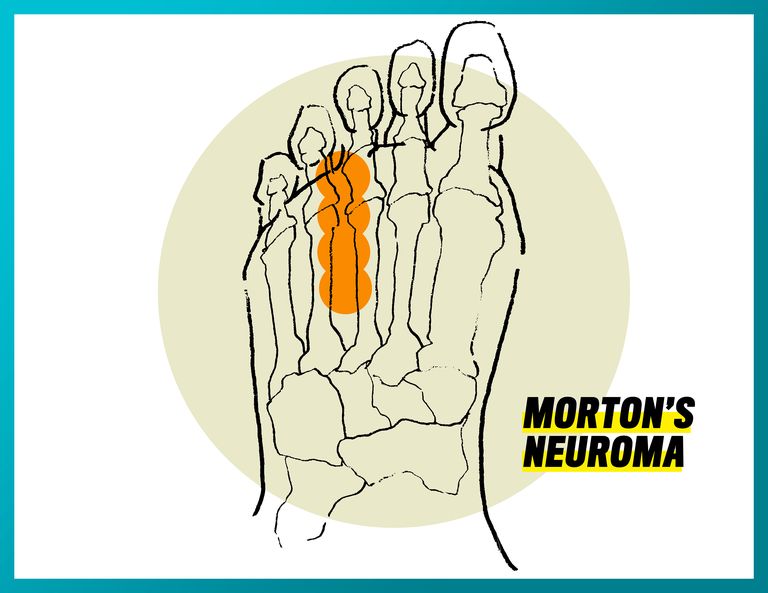
What it is: An inflammation of a bundle of nerves between the metatarsals.
What it feels like: A burning pain between the metatarsals, down by the ball of your foot. Because it’s nerve pain, the pain can radiate into your toes and cause tingling and numbness. Some equate the feeling to standing on a pebble.
What causes it: Morton’s neuroma is an inflammation of a bundle of nerves between the metatarsals, which is caused by overtraining, weak feet, and tight and/or high-heeled shoes. It can also result from constant trauma to that area of the foot (i.e., where your foot strikes when you run).
Treatment/Prevention: Check your running shoes. Are the midsoles worn? Have they surpassed their mileage? Perhaps you need a more supportive shoe. You may consider getting wider shoes, which will allow your feet to spread, with a lower stack height in the heel. You can temporarily use an over-the-counter device, like a Dr. Scholl’s metatarsal pad, to support the area. Though cortisone shots are another option to reduce inflammation, the pain may return—or remain in some cases, when the injection doesn’t work.
Posterior Tibial Tendinitis
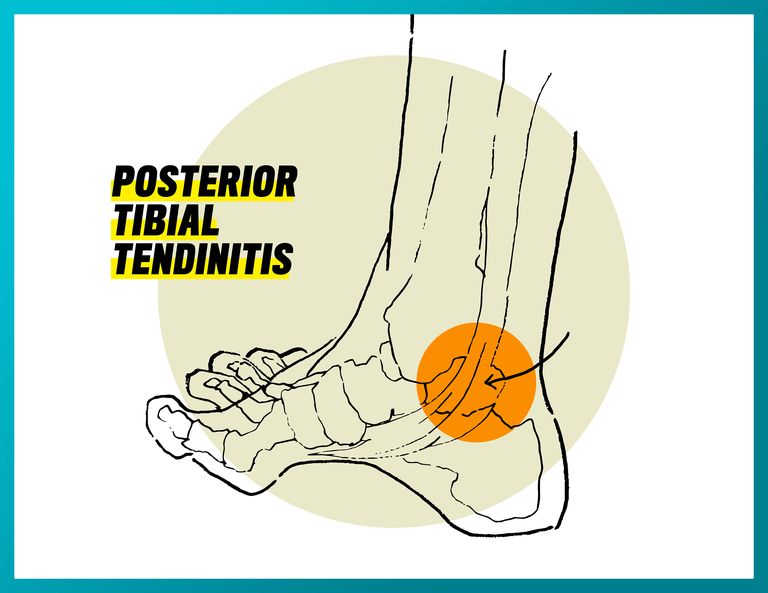
What it feels like: Pain along the inner side of the foot and ankle, as well as pain on the lateral side of the ankle from added pressure due to your heel bone shifting.
What causes it: The posterior tibial muscle is located on the inside back of the leg and comes down to the lateral side of the ankle bone and under the foot. Posterior tibial tendinitis is when this tendon becomes inflamed or torn due to overloading (a.k.a. overtraining) the posterior tib. It’s more prevalent in supinators and runners with high arches.
Treatment/prevention: Ice and rest for immediate treatment. You may need to use a walking boot, brace, or orthotic to prevent escalating the injury. Practice towel stretches, such as sitting on the ground with the injured leg stretched out in front of you and looping a towel around the ball of your foot, gently pulling the ends for 15 to 30 seconds; heel raises, and calf stretches for preventative measures.
Peroneal Tendinitis
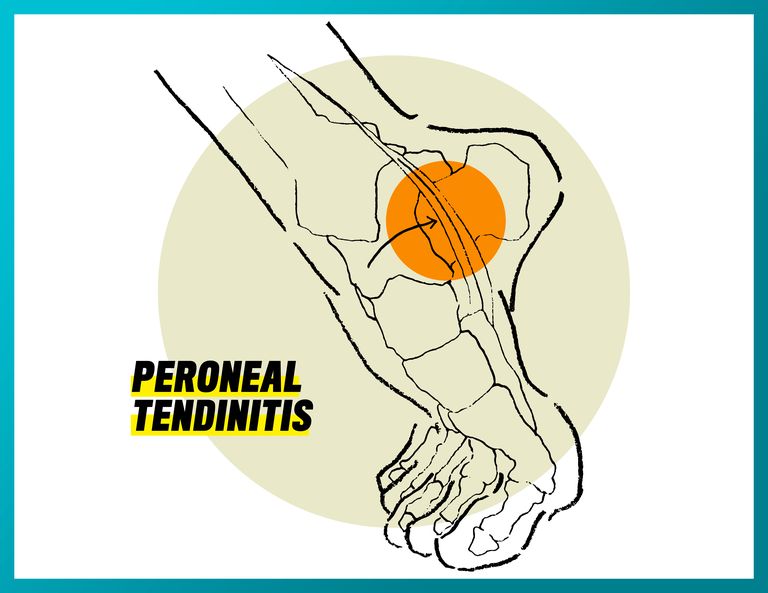
What it feels like: Pain on the outside of the ankle that worsens during running. There may also be swelling and warmth-to-the-touch at the site.
What causes it: The peroneal tendons are on the outside of the ankle behind the fibula, or calf bone. The peroneus longus tendon grooves behind the fibula and runs underneath the foot, connecting to the first metatarsal. The peroneal brevis is the shorter tendon and connects to the fifth metatarsal. Footwear that doesn’t support your feet properly, and unstable ankles can cause the tendon to become irritated.
Treatment/Prevention: Getting fitted in more supportive shoes, as well as rest for three to four weeks and anti-inflammatories can ease peroneal tendinitis. Complications with tears from an ankle injury may require a longer recovery period.
Achilles Tendinitis
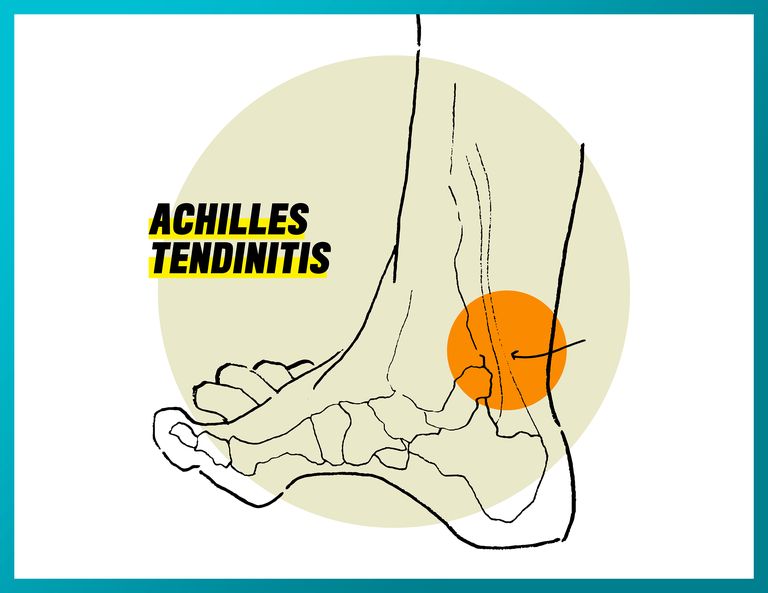
What it feels like: It begins as a mild ache on the back of the leg or above the heel, and can also manifest as a sharp pain, which can become more acute if ignored
What causes it: The Achilles tendon is the largest tendon in the body, which connects the gastrocnemius, or the calf muscle, to the calcaneus, or heel. It is the source of power behind foot push off. Achilles tendinitis is a common overuse injury that happens when you increase intensity in your training (run at a faster tempo or increase mileage drastically), and the repetitive pulling at the site of attachment gets fired up. Additionally, tight or fatigued calf muscles can cause this injury.
Treatment/Prevention: Because of its role in your foot’s biomechanics, the Achilles takes awhile to heal when it becomes inflamed, which is why early detection is important. That annoying pain above your heel? Time to throw in the towel. It can take four to six weeks to start feeling better, and up to six months of recovery if you’re not smart about giving it a rest early on, says Evans.
“It’s better to get it early,” she says. “Once you start feeling it, you need to really stop running or whatever activities are making it worse, and start rehabbing it.”
Ice and rest are a must, but you should also work in foot core exercises, and calf stretching and strengthening. Foam roll your calf to loosen muscle tightness and fit in cross-training so you don’t overload your Achilles through overuse.
Bunions
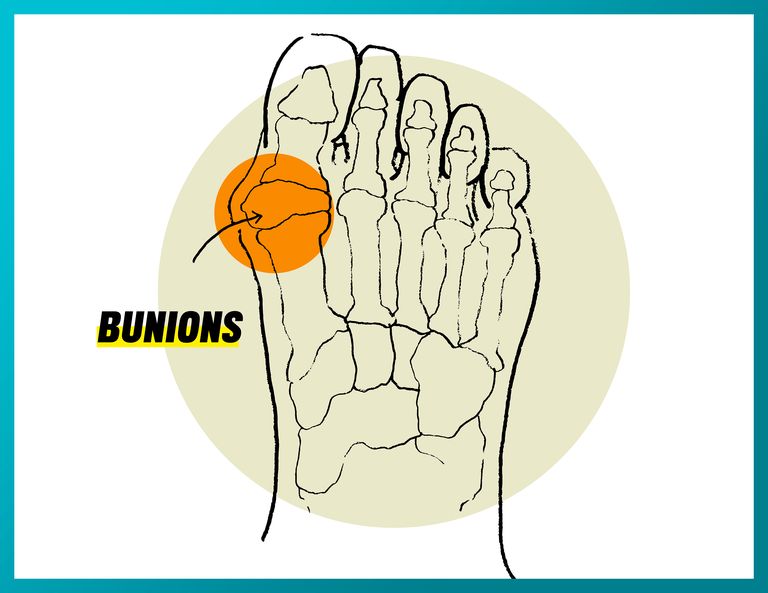
What it feels like: A sore and inflamed bump; the pain exacerbates when wearing tight footwear. You can see it develop as a calloused bump on your foot, usually on the side below your big toe or on the side of your little toe (a.k.a. tailor’s bunion). If a bunion develops, it can also cause you to unconsciously shift your stride, leading to pain in the big toe, little toe, or ball of your foot.
What causes it: The joints in your foot move out of place, causing the tip of your big toe, for instance, to pull toward your smaller toes. This causes the joint to stick out and form a bony bump. Bunions can be caused by too-narrow footwear and genetics, as well as weakened arches.
“You’ll also see it in people who don’t have good arch support,” says Evans. “The ligaments in your arch weaken just because they do with time, and the valgus, or the bunion, becomes more prominent. So having good supportive shoes that are appropriate for the type of arch that you have can really help slow down that progression.”
Treatment/Prevention: Running shoes with a wider toe box and padded socks, such as OS1st BR4 Bunion Relief Socks, can alleviate bunion pain. Drugstore gel-filled pads or moleskin can also create a cushioned buffer in your shoes. Additionally, if you wear high heels, you’ll need to take a break, as they force your toes into the front of the shoe. If the pain becomes unbearable, you may want to talk with your doctor about bunion correctors, injections or, possibly surgery.
Metatarsalgia
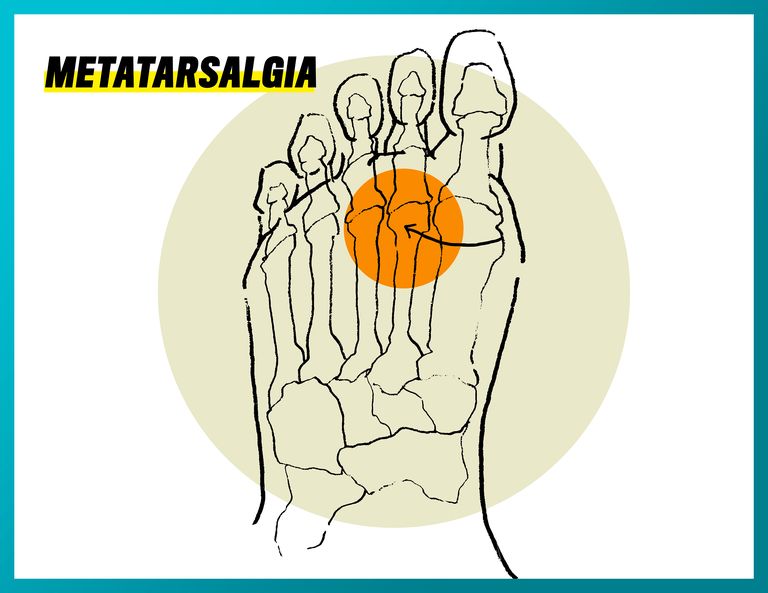
What it feels like: Pain in the ball of your foot that can sometimes feel like you’re stepping on a pebble.
What causes it: Metatarsalgia is inflammation of the metatarsals. It’s common in runners with high arches because the muscles on top of the arch tend to pull forward, making the metatarsal heads (the ball of your foot) more exposed. Age is another factor. As you get older and the fatty pad of your foot starts to thin, you become more at risk inflaming your metatarsals. Pregnancy can also cause the cushioning beneath your feet to thin.
Treatment/Prevention: Ice and rest. And foot strengthening exercises, such as grabbing a towel with your toes and scrunching it. (Do you see a pattern yet?)
Accessory Navicular Ankle Syndrome
What it feels like: A throbbing ache below your ankle on the accessory navicular bone, which is an extra bone on the medial side of your foot above the arch.
What causes it: A little bony bump like a miniature second ankle bone on the side of your foot, above your arch. Redness and swelling during and after running occurs from tight footwear rubbing against the bone. The pain can radiate across the area, causing soreness in your ankle and arch. Overtraining and trauma, such as an ankle sprain, can also cause accessory navicular ankle syndrome. Not everyone has this extra bone, and not everyone who has it will experience this condition.
Treatment/Prevention: Ice to reduce swelling. And rest. A walking boot may be required for severe cases. Corn sticker pads can be used on the bone as cushioning in narrower shoes. Extreme cases may also require surgery.
On Recovery
You’ll see us reverberate below how most injuries are caused by overtraining and not giving your body proper rest and recovery—the first step in becoming better is rest. Like Davis says, pain is a warning sign to stop what you’re doing. Even if you’re capable of running, continuing to do so can cause the pain to be chronic, or worse, exacerbate the injury.
Besides resting (and we’re talking weeks, not days), you’ll want to ice the injury to bring down inflammation, suggests Davis. Apply an ice pack covered with a towel to the injured area in increments of 15 to 20 minutes every two to three hours.
On Prevention
Incorporating foot core and calf strengthening exercises, along with resistance band stretches, into your training will help prevent injuries from recurring. Below are a some expert-suggested exercises to strengthen and stretch your feet and calves.
“I think [runners] need to be more well-rounded,” Davis says, emphasizing the importance of loading your bones in a multi-directional fashion. “It’s healthier for all of us to do activities that involve not just straight-forward motion.”